Residency Program
Endovascular Neurosurgery
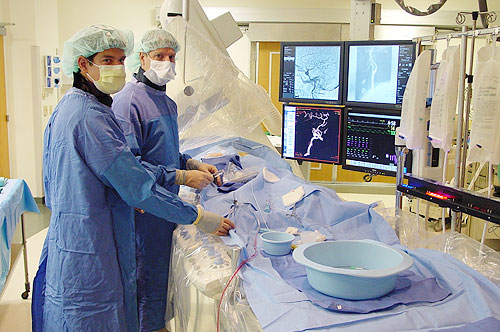
At UW Hospital, interventional radiology is managed by two fellowship trained co-directors, one from Radiology (Dr. Beverly Aagaard-Kienitz), the other from Neurosurgery (Dr. David Niemann.) This arrangement reflects the close working ties which exist between the two Departments. For neurosurgery residents in the PGY-2 year (and as time permits during PGY 4 & 5), this means that they have introductory training in angiography and transcather interventional procedures. In the PGY-6 year our resident may also elect to have a three month endovascular minifellowship for additional training. During academic year 2016-17, 357 endovascular therapeutic procedures and over 754 additional angiograms (for vascular diagnosis or for spasmolytic drug therapy) were performed by our faculty – often with the participation of neurosurgery residents.
Work Hours and Education
Our training program is designed to educate residents with minimal dilution from non–educational tasks. Although we have been granted 88 hour work week status (for PGY 2-5), no resident time is used for patient support services such as filling out request forms, phlebotomy, IV insertion, laboratory services or patient escort. No resident time is used for radiological film retrieval since online retrieval is commonly available. No time is spent responding to routine daytime patient telephone inquiries, setting up outpatient appointments, or setting up routine admissions. Our department employs nurses and nurse practitioners for these purposes.

Spectrum of Surgical Training
Residents receive training in the full spectrum of general neurosurgical problems. In addition they receive an excellent background in cerebrovascular and endovascular surgery, image guided cerebral and spinal surgery, skull based surgery, epilepsy surgery, pediatric surgery, a wide range of spine cases including complex stabilization, and stereotaxic procedures to control movement disorders. An innovative aspect of our program is the mini–fellowship that is built into the PG–6 year as an Elective Rotation.
Combined UW Hospital and VA Facilities
The William S Middleton Veteran’s Administration Hospital and the UW Hospital are physically joined. The neurosurgical faculty is the same for both hospitals and the two neurosurgical services function as a single unit. UW Hospital serves as a level one trauma and spinal cord injury center as well as a state-designated tertiary care center for nontraumatic disease. It has two Med Flight helicopters. In combination, the VA and UW hospitals have multiple in–house MRI facilities, multiple CT scanners, a positron emission tomographic scanner, a 133X3 cerebral blood flow laboratory, state–of–the–art neurovascular and MRI facilities, including a dedicated MRI-OR, and stand at the forefront in the development of MRI spectroscopy, functional MRI, 3D and perfusion / diffusion imaging.

